top of page
P O R T F O L I O O F D E V E N D R A S H E N D E - L E A D U S E R E X P E R I E N C E A R C H I T E C T / S P E C I A L I S T

This project examines the potential of AI to improve usability, streamline workflows, and deliver more intelligent digital experiences.
AI Chatbot Interface
With real provider prompts, AI responses, and embedded action cards.
How does the AI work?
The provider never has to think "where is the AI?" — it's woven into every touchpoint of their day, from the morning push notification through to the evening payout confirmation. That invisibility is the design goal: AI as infrastructure, not as a feature you have to find.

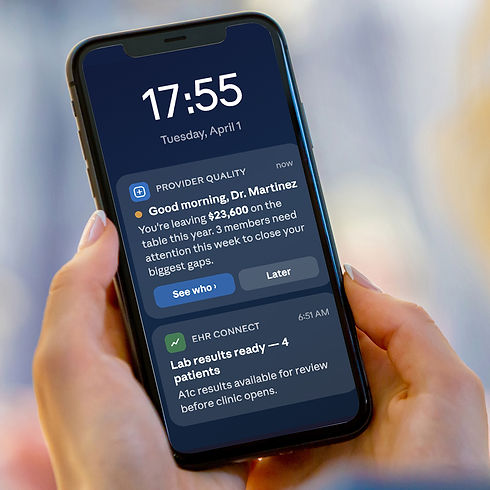
Morning Lock Screen
The phone lights up with a push notification from the Provider Quality app. The AI has already done the analysis overnight: it knows Dr. Martinez has $23,600 unclaimed, has identified the 3 highest-priority members to contact this week, and surfaces that number immediately.
Personal AI Cards
The provider opens the app and sees a personalized AI card first — not a generic dashboard. The unclaimed incentive number counts up from zero, making the financial stake visceral.
The card uses color to encode urgency — red for the most critical (A1c at 38%), amber for moderate.
Two CTAs:
1. See Priority Members
2. Straight to the 90-day plan

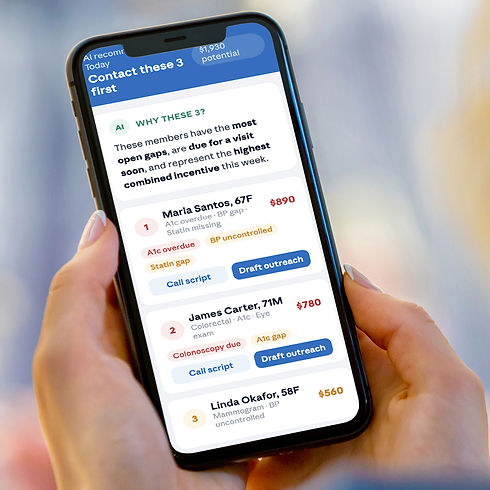
Why these 3 Priority Members?
The AI surfaces exactly three members for today, ranked by combined impact. Each card shows the member's name, open gap badges, and the incentive value tied to closing their gaps.
"Draft outreach" and "Call script" buttons are right there — the provider can act in under 30 seconds without leaving the app.
90-day plan snapshot
For the provider who wants the bigger picture, the AI shows exactly how far the current trajectory falls short of the 4.0 target
The two highest-ROI quick wins for this month
and a projected payout bar comparing current earnings ($18,400) against what's achievable by June 30 ($36,200).
The gap between those numbers is the motivation to act.


bottom of page